Features and Stories
Dig deeper into our culture of research and education by exploring some of our latest stories and features.
Research
Research is at the heart of the academics, and the goal for all of our research is to improve the health of our patients and communities.
-

Celebrating Collaborative Research in Innovation Districts
Events highlighted how Advocate Health’s Innovation Districts bring researchers, clinicians and students together to advance patient care.
-

Maternal Health to Alzheimer’s Prevention
New research shaping care across the Midwest
-

Discovery in Action
Atrium Health Wake Forest Baptist and Wake Forest University School of Medicine are celebrating the Year of Discovery as our organizational theme.
-

Measuring Impacts One Race at a Time
Joel Stitzel, PhD, professor of Biomedical Engineering, and his research team are leading the race to improve driver safety in NASCAR and other motorsports.
-

Medicine and the Military
Timothy Sell, PhD, PT, has been awarded $4.5 million from the Department of Defense to better understand and provide recommendations on injury prevention through physical interventions and equipment modifications.
-

Fifty Years of Recognized Expertise in Cancer Research
Atrium Health Wake Forest Baptist Comprehensive Cancer Center celebrates 50 years of NCI designation.
-

Researchers TEAM Up to Better Manage Blood Pressure
Cheryl D. Bushnell, MD, leads team granted $29.9 million to study ways to improve post-acute stroke care, secondary prevention.
-

AI: The Future of Health Care
Metin Nafi Gurcan, PhD, leads the Center for Artificial Intelligence Research to serve as a trusted partner and advise on the role of AI in medicine.
-

Infants and Older Adults May Hold Key to More Effective Vaccines
Martha Alexander-Miller, PhD, and the research team at the Center for Vaccines at the Extremes of Aging look for answers.
-

Keeping Youth Athletes Safe
Joel Stitzel, PhD, and Jillian Urban, PhD, are pioneering research that improves the safety of youth football on and off the field.
-

Zombies: Are They Already in Your Head?
Miranda Orr, PhD, is examining the role of senescent “zombie” cells in brain disease and how they impact Alzheimer’s Disease research.
-

RegeneratOR Test Bed Provides Access to Emerging Technology
Leaders in regenerative medicine provide free space and a state-of-the-art facility for companies to advance discoveries.
-

Community Partnership to Improve Cancer Care
$25 million grant helps researchers bring cancer clinical trials and care delivery studies to people in their communities.
-

Scientists and Students Study the Risks of Space Travel
Researchers at the Jeffrey Willey Lab are working with NASA to utilize new tactics, approaches and exploration quests to keep astronauts safe and healthy throughout their missions.
-

Advancing Care for Stroke Patients
Researchers created the Comprehensive Post-Acute Stroke Services study, the first statewide study to improve care and resources after a stroke.
-

Performance Research Gets You Back on Your Feet
Atrium Health clinicians and researchers created the innovative Return to Performance Pathway Program to get people back to their desired physical activities in under six weeks.
-

Regular Blood Pressure Checks Can Save Your Life
Our researchers discovered that lowering blood pressure is the first intervention in history to also reduce the risk for memory loss, in addition to heart attacks and strokes.
-

Youth Sports Research Scores Points with Parents
Our researchers spearheaded a first-of-its-kind youth football head injury study that has helped make youth sports safer.
-

Cracking the Code to Discover Risks of Alzheimer’s Disease
Our researchers are joining forces to develop screening tools and study biomarkers to help solve the puzzle of Alzheimer’s disease.
-

Improved Outcomes for Children Exposed to Opioids Before Birth
Our researchers are addressing the ongoing medical and developmental needs of children born with Neonatal Abstinence Syndrome.
-

Regenerative Medicine Takes Research to Galactic Heights with NASA
WFIRM is working with NASA to accelerate engineering innovations and strategies for making tissues with artificial blood vessels, as well as health risks astronauts face during missions in deep space.
-

CUPID Research: Finding Faster Ways to Pinpoint the Deadliest Strokes
Researchers at Wake Forest University School of Medicine and Atrium Health received pilot funding to collaborate and improve patient care.
-

Walk On! Research Project Takes Leap Forward
Program increases chances to improve mobility and reduce social isolation in older adults thanks to partners at Atrium Health and new funding from The Duke Endowment.
-

On the mPATH to Better Health and Longer Lives
Researchers place the power of health screenings directly in patients' hands.
-

Walk On! Research Project Takes Leap Forward
Program increases chances to improve mobility and reduce social isolation in older adults thanks to partners at Atrium Health and new funding from The Duke Endowment.
-

On the mPATH to Better Health and Longer Lives
Researchers place the power of health screenings directly in patients' hands.
-

Mask Shortages and Innovative Collaboration
How do we create a better mask? Philip Brown, PhD, assistant professor of Biomedical Engineering at Wake Forest School of Medicine is looking to do just that.
-

School Leaders Honor Veterans Health Administration
School faculty reflect on the school's affiliation with the W.G. (Bill) Hefner VA Medical Center in Salisbury in celebration of the Veterans Health Administration 75th anniversary.
-

HEART Pathway
Revolutionary clinical algorithm for risk stratification of patients who present with chest pain has evolved capabilities and expanded influence since its 2016 release.
-

A Geriatrician at Your Fingertips
Read how our new predictive tool, Electronic Frailty Index (eFI), enhances health care and quality of life outcomes for older adults.
-

Closing the Gap: The IGLOO Story
Wake Forest demonstrates how a health care system can more quickly turn research outcomes into patient care with a new blood pressure measurement protocol that may help prevent strokes and cardiovascular events.
-

Decoding Vaccine Trials
As COVID-19 vaccines are introduced to the public, a few of our biostatistics experts explain the basic design of a vaccine trial and how we determine whether a vaccine is safe.
-

Positioned for Progress: Cancer Biology at Wake Forest Baptist
Wake Forest School of Medicine's cancer biology research team works to move cancer research forward, from cell culture to experimental animal models to human patients.
-

Seeking Solutions
Wake Forest researchers are collaborating across the organization to combat the opioid crisis by investing in a range of programs and continuing rigorous research.
-

Using Noninvasive Brainwave Technology to Treat PTSD Symptoms
Researchers test noninvasive brainwave technology to see if it would help military veterans who report experiencing symptoms of post-traumatic stress disorder.
-

Building a Better Body on a Chip
Scientists create micro-sized 3D organ structures on chip to test how organ systems react to aid drug development process.
-

Data Networks Power COVID Research
Wake Forest School of Medicine researchers are contributing to the development of powerful new data networks that will provide important new information in the quest to conquer COVID-19.
Education
We offer innovative programs to educate the next generation of health care leaders, and invite learners of all ages and backgrounds to join us in our pursuit of excellence.
-

White Coats Run in the Family
For Mattie Harris and Zach Harris, medicine became more than a career path — it became a family bond.
-

Local High School Students Explore Future Health Care Careers at MEDucation Day 2026
High school juniors in the Winston-Salem and Charlotte areas discover health care advancements and career opportunities at Advocate Health.
-

Brains, Bones and Bragging Rights: The Anatomy Cup Debuts at The Pearl
Meet Dr. Tafline Arbor, an anatomy educator who is redefining how students experience learning.
-

Clearer Vision, Safer Lives: A Student-Led Effort Expands Access to Eye Care
Wake Forest University School of Medicine students provide free community eye health screenings.
-

Match Day Started it All
Class of 2002 alumni, high school sweethearts and longtime faculty members, Sarah and Mike Cartwright, M.D., reflect on their Match Day experience
-

A Childhood Cancer Diagnosis Sparked His Dream, Match Day Made it Real
Kameron Williamson reflects on Match Day, residency and the childhood experience that inspired his calling
-

AHWFB Hosts Neurology Mentorship Program for Local High School Students
Atrium Health Wake Forest Baptist recently hosted 40 high school students from Winston-Salem/Forsyth County Schools’ Department of Career and Technical Education for a neurology mentorship program.
-

Charlotte Campus Opens for Medical Students
School of Medicine MD Program faculty and staff officially moved into The Pearl Innovation District in Charlotte.
-

Charlotte Campus Students Take Community Orientation Bus Ride
Third-year medical students at the Charlotte campus participated in a community orientation bus ride of the Queen City which provided a location overview of where some of the most medically complex patients live and work.
-

RxPurpose: Medical Students Providing Hope
RxPurpose is a food recovery initiative, spearheaded by medical students, that distributes excess and unprepared hospital food to The Salvation Army Center of Hope Family Shelter which provides hot meals for 50+ shelter guests each week.
-

Medical Student's Health Journey Comes Full Circle
Sydney Karre has created a pipeline for her peers to support the Ronald McDonald House.
-

Celebrating 50 Years of Northwest AHEC
Northwest AHEC serves as a primary resource for educational activities and services with a focus on primary care in rural communities and areas with less access to resources.
-

Mentorship and Collaboration in Research
The Solberg Woods Lab is composed of researchers at varying levels of their careers.
-

Charlotte Campus Progress in the Pearl
Wake Forest University School of Medicine’s second campus in Charlotte combines health care education and technology.
-

Medical Students Enhancing Global Health
Certificate program prepares medical students to understand emerging health challenges.
-

Ultrasound Course Prepares Students to Save Lives
Campbell Veasey, MD Class of 2024, was able to help save a patient thanks to specialized education.
-

Journey from Haiti to Medical School
Vanessa Camille experienced two TBIs during her late teens and was exposed to both good and bad clinicians which ignited her passion and goal to pursue medicine.
-

Teaching Compassionate Care
Dalane Kitzman, MD, advises students that compassion makes the difference in providing patient care.
-

Summer in the City: Students Get Innovative Experiences
The School of Medicine provides STEM and health care education programs for middle and high school-aged children, as well as internship opportunities for future researchers.
-

Home Sweet Home
How Learning Communities – also known as Houses – provide support for medical students.
-

Graduate School Alumni Making a Difference
From discovering the benefits to melatonin, to working at the NIH on ways to solve the mysteries of the brain and nervous system – learn how our alumni have improved health.
-

Training the Next Generation of Scientists
Educating students and trainees on ways to improve patients' lives through regenerative medicine.
-

The Doctor is In: Residency and Fellowship Opportunities
With nine research centers funded by the NIH, over 3,500 research projects and more than $319 million in research funding, there are extensive research possibilities for trainees.
-

Radiology Scholarly Program Teaches Critical Skills
Addressing deficits in radiology education and offering students exposure to the radiology field during preclinical years.
-

Integrating Lifestyle and Integrative Medicine
Scholarly program educates students on non-traditional ways to counsel patients with pain, chronic disease and mental health.
-

Medical Students Collect 600+ Prescription Glasses for Communities in Need
Students participating in Respectacle help collect and repurpose donated prescription glasses for those who may be struggling to obtain them through conventional means.
-

The ART of Managing Medical School Stress
The Active Resilience Training in Medicine program provides medical students with prevention-focused tactics to promote wellness and alleviate or prevent anxiety and burnout.
-

Medical Students Help Kids Become their Best SELF
Our medical students provide academic mentorship for middle and high school-aged children.
-

Program Teaches Future Clinicians How to Be Good Educators
Discover how one of Wake Forest’s Programs of Distinction provides medical, physician assistant (PA), and nurse anesthetist students a unique opportunity to gain focused training in medical education in an interprofessional setting.
-

Wilderness Medicine: Where the Wild Things Are
Wilderness Medicine Concentration offers students an introduction to wilderness and austere medical care.
-

Camp Med Teaches Life-Saving Skills to Future Health Care Professionals
A high school student recently saved his friend from choking after completing Camp Med training.
-

Cultivating Tomorrow’s Leaders in Health Care
Read how the Wake Forest Interprofessional Leaders in Health Care (ILHC) program helps students identify their personal leadership style and build the confidence and esteem in their future careers.
-

Learning While Serving
The Service-Learning Scholars (SLS) scholarly program helps students develop the awareness and skills they need to become community partners and advocates.
-
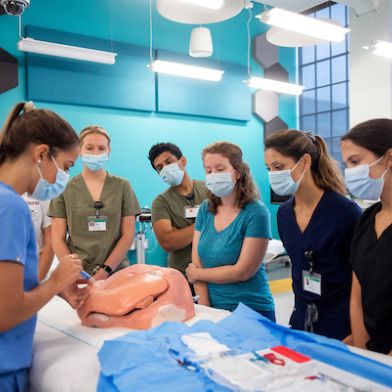
CEAL Educates Wake Forest School of Medicine Students
The Center for Experiential and Applied Learning (CEAL) provides advanced medical school teaching facilities to improve clinical education for students and providers.
-

Four Reasons to Get Your DNP Degree at a School of Medicine
Across the country, only a handful of DNP programs are offered by Schools of Medicine. Here are four advantages to getting a DNP from a School of Medicine.
-

Creating Agents of Change in the Opioid Epidemic
Opioid stewardship training empowers medical students to address addiction and pain management.
-

Practice Makes Perfect
New accreditations recognize our innovative use of simulations to equip the next generation of health professionals.
Profiles
Meet the people who make a difference in our community through research, education and innovation.
-

Bridging Biomechanics to Baseball
Kristen Nicholson, PhD, oversees data collection, research and biomechanics interpretation at the Wake Forest Pitching Lab – her goal is to understand pitching efficiency and the ability to reduce injury risk while maximizing performance.
-

Medicine Takes Flight
Thomas Marshburn, MD, graduated from the School of Medicine in 1989 and is an astronaut veteran of three NASA spaceflights.
-

Breast Cancer Research: From Bench to Bedside
Marissa Howard-McNatt, MD, is one of the few African-American female surgeons who have full professorships in the country; as a surgical breast oncologist she’s hoping to inspire the next generation of female surgeons.
-

Shaping the Future: One School, One Mission, Two Campuses
Dr. Michele Birch is developing and implementing the curriculum at Wake Forest University School of Medicine's Charlotte campus to ensure future medical students achieve excellence.
-

Michael Shapiro
Michael Shapiro, DO, MCR, is at the forefront of preventive cardiology and combines traditional methods with new approaches based on research to prevent heart disease.
-

Disease Prevention: Diet and Exercise as Medicine
Tina Brinkley, PhD, is providing research that showcases how nutrition and activity can prevent and treat aging-related diseases.
-

Research Exploration: From Genetic Disorders to NASA Wellness
The Porada Lab is advancing and improving the outlook of genetic disorders and progressing the wellness of NASA astronauts.
-

Discovery for All: Innovative Research Monitors Vital Signs of Patients in the ICU
Ashish Khanna, MD, merges his research to improve clinical care with his digital expertise in wireless monitoring technology, hemodynamics, vasopressors and artificial intelligence with a touch of amateur podcasting.
-

In Their Own Words: Modupeola Akinola, MBBS
Learn how this Assistant Dean of Admissions and Associate Professor of Pediatrics-Neonatology balances her time between recruiting, teaching and mentoring students while caring for The Birth Center’s tiniest patients.
-

In Their Own Words: Jason Stopyra, MD
Learn how this Associate Professor of Emergency Medicine and Medical Director for Randolph and Iredell County EMS works to address healthcare in rural communities.
-

In Their Own Words: Tiffany Shin, MD
Learn how the director of the MAESTRO Program prepares students to become comprehensive healthcare professionals.
-

In Their Own Words: Metin N. Gurcan, PhD
Learn how the director of the Center for Biomedical Informatics leverages data to advance healthcare technologies and why he believes the power of science can help reduce suffering around the world.
-

Sara R. Jones, PhD
Sara R. Jones, PhD, is on a mission to cure substance use disorders. Her various leadership roles, including chair of the Department of Translational Neuroscience, help her harness the combined research power of Wake Forest University School of Medicine’s substance use experts to make an impact.
-

In Their Own Words: Yenya Hu, MD, PhD
Hear from the Wake Forest University School of Medicine’s assistant dean of academic excellence and support about her passion for helping future physicians achieve their personal goals and reach their full potential.
-

Candace Parker-Autry, MD
Candace Parker-Autry, MD, assistant professor of Urology, was inspired by her grandmother’s experiences to find ways to improve the daily life and function for women impacted by incontinence.
-

Kerry Danelson, PhD
Kerry Danelson, PhD, associate professor of orthopaedic surgery, leverages her former military training and service in conducting military safety and orthopaedic biomechanical testing to reduce the risk of injury for other service members.
-

In Their Own Words: Paul Yelton
Hear straight from Paul Yelton, program director of technology for the Center for Healthcare Innovation, why he is passionate to bring the best technology to transform the way we deliver care to our patients.
-

Rebecca Wells, MD, MPH
When Rebecca Wells, MD, MPH, started medical school she thought she wanted to be a pediatrician, but a curiosity about the mind-body connection ultimately led her in a different direction.
-

Faculty in Focus: Joey Skelton, MD
Joey Skelton, MD, a researcher, clinician and educator, has a passion for food and keeping children healthy, leading to groundbreaking work in pediatric obesity.
-

Jamy Ard, MD
Jamy Ard, MD, helps people lose weight and improve their health in the clinic and through his research.
-

Faculty in Focus: Chris Miles, MD
Chris Miles, MD, a researcher, clinician and educator at Wake Forest School of Medicine, has a passion for the medicine of exercise, leading to groundbreaking work to make sports safer.
-

On the Frontlines
Wake Forest University School of Medicine grad Matt Russell, PA-C, shares his experiences working at the epicenter of New York City's first wave of the novel coronavirus.
Awards and Recognition
The work and dedication of our faculty, staff and students enhance the Wake Forest University School of Medicine’s reputation. Read about some of the national and international awards and recognition they have earned, their grants and published research, and their achievements.
Milestones
Wake Forest University School of Medicine celebrates pivotal events and achievements throughout the year.


Keep Up with Wake Forest University School of Medicine
If you have enjoyed one or more of the features found here and would like to read more and stay on top of life at Wake Forest University School of Medicine, please join our subscriber list.






