Although less than one in five strokes are caused by intracerebral hemorrhage (ICH), or bleeding in the brain, this type of stroke is the deadliest. A new study led by Aarti Sarwal, MD, professor of neurology at Wake Forest University School of Medicine, is examining whether it is possible to identify patients with an ICH stroke before they get to the hospital in order to help these patients get life-saving care without delay.
“For ICH, outcomes tend to be much worse if patients get specialized care more than six hours after onset,” said Sarwal. “Patients in rural areas, or who are minorities, are disproportionately affected because they may be hesitant to go to the hospital due to cost or other factors. Also, time might be lost when they are taken to a regional hospital and then transferred to a specialized center.”
The study is supported by the National Institutes of Health-funded Wake Forest Clinical and Translational Science Institute (CTSI) Strategic Combination Joint Pilot Program. This program encourages the development of interdisciplinary research teams for translational research involving collaborators across the new Atrium Health Enterprise.
“With Atrium Health and Wake Forest Baptist now being one enterprise, we've brought the best forces in healthcare management together,” said research team member Pamela W. Duncan, PhD, professor of neurology at Wake Forest University School of Medicine. “We are combining the excellent research capabilities of the school of medicine’s Department of Neurology with the clinical enterprise to more rapidly influence frontline clinical care and bring more patients the opportunity to benefit from research.”
Identifying brain bleeds
Determining which patients have ICH before they get to the hospital would allow them to be routed directly to a more advanced hospital with the capability to treat stroke patients, even if it isn’t the closest. This is particularly important in rural areas because it may mean driving a little bit longer or crossing a county line to get to the right hospital. Paramedics could also administer agents that can slow the bleeding before the patient even gets to the hospital.
“During these critical early hours, people with ICH are typically in transit, where they are getting worse and not coming to specialized care,” explained Sarwal. “Right now, we don’t know that they have a bleeding stroke until they have a CT scan in the emergency department.”
| “During these critical early hours, people with ICH are typically in transit, where they are getting worse and not coming to specialized care. Right now, we don’t know that they have a bleeding stroke until they have a CT scan in the emergency department.” - Aarti Sarwal, MD | 
|
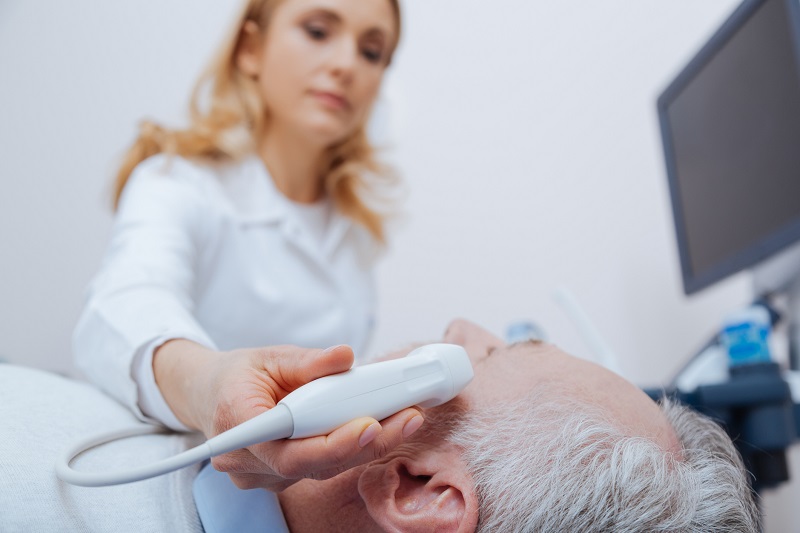
For the new pilot study, which is called CUPID: Cranial Ultrasound for Prehospital ICH Diagnosis, Sarwal and her team are testing whether paramedics could use hand-held ultrasound devices to identify ICH cases. New technology has made ultrasound machines more portable and easier to use. The idea behind the study is that paramedics could use these devices in the field and then securely send the images to physicians for real-time interpretation.
Duncan, a senior researcher with years of experience designing and conducting successful research trials, is serving as Sarwal’s mentor on this study. She understands firsthand what a difference quick actions have when it comes to a brain bleed.
“I experienced two ICH bleeds from trauma after an accident,” said Duncan. “Because it was immediately known that I had ICH bleeds, the appropriate therapies were started, and I was immediately transported to a tertiary care center. They were able to control the bleeding, and I am speaking to you today as a perfectly recovered person because of this care.”
Will it work?
The first part of the CUPID study aims to determine whether ultrasound can be used to pinpoint a stroke caused by a brain bleed. For this, an ultrasound is performed on ICU patients who have received a head CT for any reason. Researchers examine the ultrasound images to determine which ones show a brain bleed, while being blinded to the CT results. Although the COVID-19 pandemic has made it more difficult to obtain the necessary consents for ICU patients to participate in this research, the team has been able to enroll about 60 patients for a total of 100 scans so far.
 |
“I experienced two ICH bleeds from trauma after an accident. They were able to control the bleeding, and I am speaking to you today as a perfectly recovered person because of this care.” - Pamela Duncan, PhD |
The second part of the study will use what is learned from the ICU study to train paramedics on how to aid ICH diagnosis in the field. Research team member Andrew Asimos, MD, from Atrium Health’s Carolinas Medical Center in Charlotte is playing an important role in this. He is an emergency medicine physician and has worked with many EMS providers while conducting research on regional acute stroke care.
“The study will also look at some of the practical aspects of diagnosing ICH before the patient gets to the hospital,” said Asimos. “For example, can the images be transmitted securely and appropriately even in areas without strong cell phone signals, and can those images be used to quickly and accurately determine if brain bleeding is present?”
Reaching rural areas
Asimos has helped connect Sarwal to rural counties that have a high number of brain bleeds compared to other counties.
“This was possible due to our partnership with Atrium Health,” said Sarwal. “Asimos has done phenomenal work on improving systems of care in ischemic stroke. Having his knowledge and expertise in designing a trial that can be implemented for hemorrhagic stroke was extremely valuable.”
Although staffing shortages related to the ongoing pandemic have made it challenging for paramedics to participate in research studies, EMS agencies in Iredell County are now undergoing training to join the study. Those in several other counties are also considering whether they can participate.
| “The combined Atrium Health and Wake Forest Baptist enterprise has greatly expanded the potential EMS agencies that can participate in this study and provides access to an incredible number of patients. It also gives patients access to trials that they would not be able to participate in if we didn't have such a big network of patients to draw from.” - Andrew Asimos, MD | 
|
Sarwal says that the CTSI pilot funding was very helpful not only because it encourages research across the enterprise but also because it is extremely challenging to secure funding for this type of study.
If the researchers are successful in finding a way to identify ICH strokes in the field, then it could provide the data needed to secure funding for more and larger studies. It would also create a way to study which pre-hospital interventions may help to keep bleeding in check and improve outcomes, which hasn’t been possible without a way to identify ICH strokes before patients get to the hospital.
