Our curriculum is highly structured. It is carefully designed to optimize skills development since anesthesiology is difficult to master and inherently dangerous. Learning theory is applied to determine how we teach because the progression of when you do things is just as important as how you do them. That which is most important is done most often, and that which is particularly difficult is approached from many angles to assure mastery.
Virtual Tour
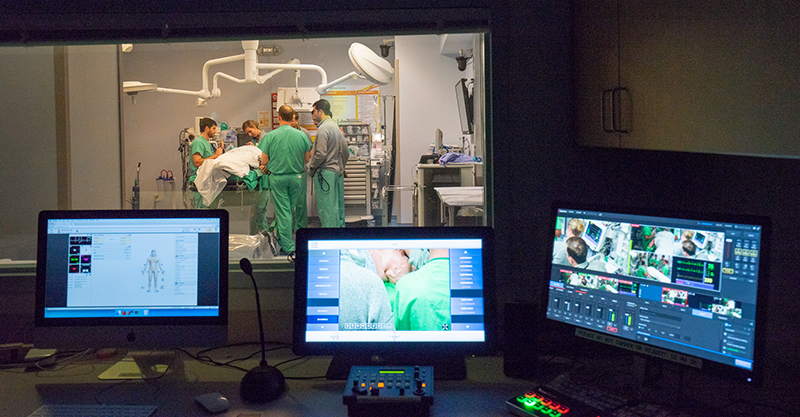
Depending on your rotation, you may train at facilities across our system. Explore below a few of the spaces where residents of this program spend a lot of their time.
Study Guide
Each of our rotations has a Study Guide to be completed that we call Things to Remember comprised of several pages of short answer questions designed by our faculty. This Study Guide is reviewed in the middle of the rotation to guarantee that everything that should be learned from that rotation is indeed covered in depth. Dozens of faculty members ensure this is accomplished for each rotation. Introductory rotations emphasize pharmacology, physiology and anatomy while our advanced rotations focus more on case planning and management. There is very little written in books about how to actually do a case, so we discuss the specifics, planning and performance of cases in depth-each and every day.

Our lecture series is similarly structured and logical in its delivery. The academic year produces its own seasons that are clearly evident in teaching centers. Each quarter we move from introductory general topics to primary subspecialties, advanced operative specialties, and ultimately the perioperative disciplines. All of our sections get 2-4 week blocks of time in one of these quarters and teach their specialty specific curriculum in a two or three year cycle. As with the Study Guides, this formal construct makes sure that everything is covered at the proper time of the academic year so it has the most impact on every class in the residency.


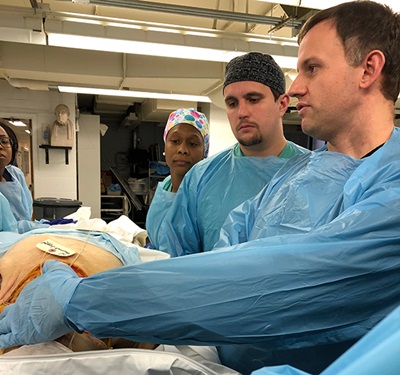 Cadaveric Workshops—An entire week each year is set aside for hands-on cadaveric workshop for upper- and lower-extremity blocks. An additional day is spent covering pertinent airway anatomy to teach airway blocks, cricothyrotomy and other advanced airway techniques such as retrograde wire intubation.
Cadaveric Workshops—An entire week each year is set aside for hands-on cadaveric workshop for upper- and lower-extremity blocks. An additional day is spent covering pertinent airway anatomy to teach airway blocks, cricothyrotomy and other advanced airway techniques such as retrograde wire intubation.