The section of Regional Anesthesia and Acute Pain Management (RAAPM) was founded in 2003 and is made up of nine board-certified anesthesiologists with fellowship training or special interest in regional anesthesia and acute pain management who work with four CA-2 or CA-3 residents rotating on service each month. The RAAPM section is responsible for the provision of regional anesthetics and acute pain management throughout our 800-plus bed inpatient hospital as well as our ambulatory surgery areas. Our department performs 15,350 blocks annually. Of this total, the RAAPM section performs almost 7,000 annually, which includes 2,000 neuraxial blocks, 3,600 peripheral nerve blocks (10 percent are continuous - i.e., nerve block catheters) and more than 1,000 truncal blocks.
Our routine practices include the use of
- Nerve stimulation catheter techniques
- Ultrasound guidance
- Epidural infusion therapies
- Ambulatory peripheral nerve block pumps
The list of surgical subspecialties for which we provide regional analgesia and/or anesthesia consist of a variety of fields, including orthopedic, gynecologic, thoracic, general surgery, vascular, surgical oncology, and many others.
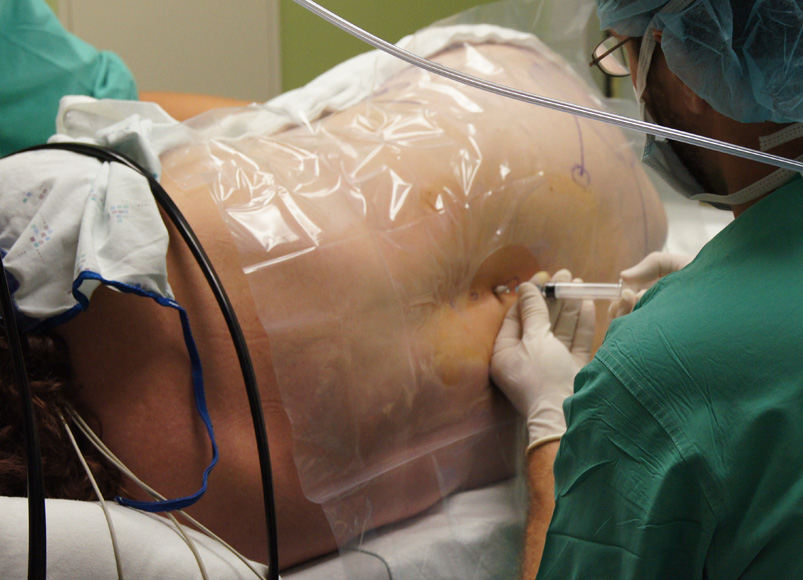
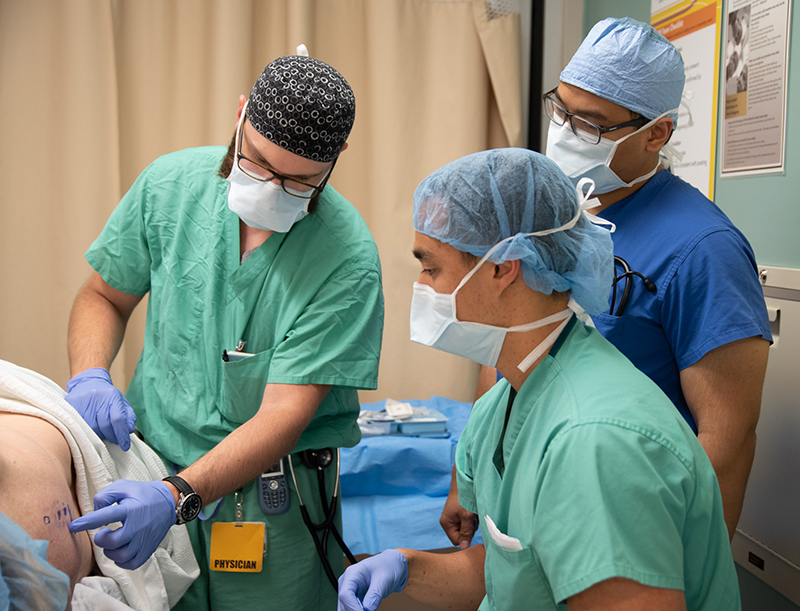
Resident education and hands-on involvement are the cornerstones of patient care in our section, and most residents perform more blocks by the end of their first month in RAAPM than are required during their entire anesthesia residency. By graduation, our residents have complete the require number of blocks (both neuraxial peripheral) multiple times.
It is our belief that residents deserve the opportunity to grow from a guided regional experience on their first rotation through RAAPM to performing blocks autonomously prior to graduation. By the time our residents finish, they are able to orchestrate their own blocks, including deciding which block and local anesthetic is best for the patient and seeing the block through to completion.
From a scholastic perspective, regional anesthesia and acute pain management are a standard part of department conferences. The RAAPM faculty members contribute to didactics both during the month's rotation and as part of the ongoing afternoon lecture series provided for all residents.
In addition to this, we provide more hands-on learning experiences through a two-day cadaver lab and simulation experiences. The hands-on education experience in RAAPM culminates in a skills evaluation where senior residents have the opportunity to take part in a simulated patient experience in preparation for the ABA OSCE. When on rotation, didactic curriculum includes a weekly subspecialty conference and a monthly journal club in which we select literature at a local restaurant.
Anesthesia residents at Wake Forest School of Medicine have at their disposal the resources necessary to leave their residency capable of providing consultant-level patient care in sophisticated techniques for acute pain management, such as thoracic epidural analgesia and continuous peripheral nerve blockade.
With regard to the breadth of regional anesthesia topics and procedures that are covered during our resident’s 3-4 months of RAAPM rotations, an abbreviated list of blocks includes:
- Interscalene
- Supraclavicular
- Infraclavicular
- Axillary
- Forearm/wrist
- Pectoralis plane (PECS)
- Rectus sheath
- Transversus abdominis plane(TAP)
- Quadratus Lumborum
- Ilioinguinal/iliohypogastric
- Lumbar plexus
- Femoral
- Obturator
- Lateral femoral cutaneous
- Adductor canal
- Anterior sciatic
- Labat and sub-gluteal sciatic
- Popliteal sciatic
- Tibial
- iPACK
- Ankle
- Paravertebral
- Erector spinae
- Spinal
- Spinal catheter
- Epidural blood patch
- Thoracic and lumbar epidural
In addition to the procedural aspect of our rotation, we also spend time teaching our residents about acute pain management. Topics of instruction in this arena include:
- Acute opiate management
- Acute pain management for chronic pain patients
- IV PCA optimization
- Methadone therapy
- Cancer pain
- Peri-neural and epidural catheter management
- Multimodal analgesia
- Trauma analgesia
- Complications of acute pain management
- Pediatric pain therapies
The RAAPM Procedural Area
All of these regional anesthetics are initiated in a dedicated, six-bay Regional Anesthesia Area staffed by specially trained nurses. Medical direction is covered by both a regional fellowship-trained attending anesthesiologist and a general anesthesiologist who have a special interest in regional anesthesia.
Postoperatively, the on-call resident manages patients using a foundation of multimodal analgesia and regional techniques. It is during this experience that residents are able to gain exposure to the management of thoracic epidurals, peripheral nerve block catheters and multimodal analgesic management. In addition to providing care for inpatients recovering from surgery, the RAAPM section also maintains an active census of outpatients managed with continuous peripheral nerve blockade at home and a small subset of chronic pain patients managed in the hospital.